Written by Steven Burns
From his column To Your Health
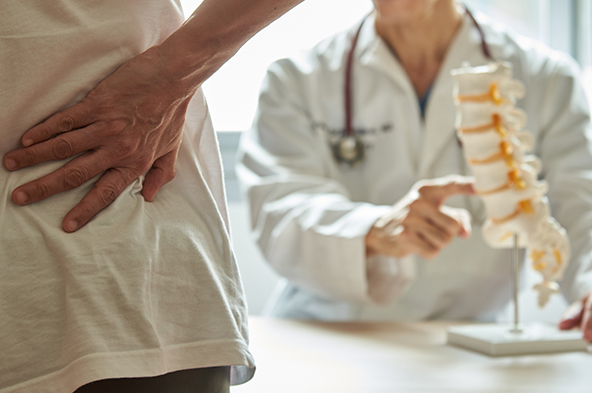 “Doc, I’m leaving town tomorrow for my daughter’s wedding, and my pills will be all gone on Saturday. They’re not due to be refilled for four days. Could you give me an early prescription so I won’t run out?”
“Doc, I’m leaving town tomorrow for my daughter’s wedding, and my pills will be all gone on Saturday. They’re not due to be refilled for four days. Could you give me an early prescription so I won’t run out?”
Bill has been my patient for a long time, has chronic pain, and has used opioid pain relievers for many years. He was in a boating accident that broke his neck, and he has had many operations. His neck is made of titanium and pain.
“Bill, you know we have a contract about the oxycodone. But you’re really careful with these meds. I’ll call the pharmacist, and we’ll fill your next prescription 4 days early. We’ll resume your usual schedule for next month.” He agreed, and I sent the prescription.
In the United States, more than 50 million adults, about 1 in 5, suffer from pain that’s been present for over 6 months. Of these, 8% have severe pain that limits their daily activities. When you’re sitting in church, realize that about a fifth of the congregation have chronic pain. The percentage of sufferers grows as people age.
You’ve probably read about the opioid crisis. In past decades, Purdue Pharmaceuticals produced massive amounts of long-acting oxycodone, marketed with the lie that it was less addictive than the short-acting pills. Many thousands of patients died as a result of addiction, overdose, and transition to illegal street drugs. Some were legitimate pain patients. Some were addicts who crushed the pills and injected them. Some faked pain to buy and then sell the pills on the street. Why would anyone prescribe such a drug?
Well, life is more messy than the news would lead us to believe. In Bill’s case, he gets 75 tablets of oxycodone with acetaminophen each month, the lowest amount of narcotic he has been on in many years. He and I have worked together to reduce his dosage, and Bill is an active partner. He does not want to take this medication. I’ve seen his x-rays. He has a lot of hardware that does not bend much at all. He has massive headaches and neck pain. He has tried many pain clinics, surgeons, and anesthesiologists, with little benefit. Epidural steroid injections do not help him. He spends his days with heat on the area, doing gentle stretches to relieve the hurt. Occasionally he gets a massage, which helps a bit.
Many family physicians have a few chronic pain patients like Bill, patients who take a set amount of narcotic pain reliever. Their pain varies, but it is always there, and it is always bad. In Bill’s case, you can see the deep scar on the back of his neck, and feel the muscle spasms on all sides of the disaster that is his spine. He has tried everything I have suggested. He is at the lowest level of opioids he can take and still live his life.
When a person develops chronic pain, we use non-steroidal anti-inflammatory drugs (NSAIDs) as first-line therapy. When used correctly, they are effective and safe, with no addictive properties. However, NSAIDs can cause ulcers and bleeding, as well as high blood pressure, kidney damage, and heart disease. Even the over-the-counter ones (aspirin, ibuprofen, naproxen) can have these effects.
When NSAIDs are not effective, other medications may be used. Anticonvulsants can relieve nerve pain, often better than narcotics. Some antidepressants have side benefits of pain relief. Muscle relaxers can help with muscle spasms. Corticosteroids can help relieve pain with acute inflammation, but side effects limit their use to short periods of time.
Physical therapy can help many types of chronic pain. Exercise is a powerful pain reliever, even when it hurts to start. Anesthesiologists can place steroids near the nerves as they exit the spine (epidurals). The steroids decrease nerve inflammation, often helping to relieve pain dramatically. Specialists in Physical Medicine and Rehabilitation also do epidurals, but more often they use physical therapy and noninvasive methods.
So, what should you do if you start experiencing severe, long-lasting pain? First, see your primary care physician. He or she can run tests to diagnose the problem and set you on the right treatment path. Unfortunately, in many cases, diagnosis can take weeks. While this is going on, work with your physician to use as little pain medicine as possible. Even small amounts of narcotics can have addictive properties. If you are already taking an opioid, your doctor may refer you to a pain specialist who can determine the best and safest treatment.
The apostle Paul knew something about pain. He said, “To keep me from becoming conceited because of these surpassingly great revelations, there was given me a thorn in my flesh, a messenger of Satan, to torment me. Three times I pleaded with the Lord to take it away from me. But he said to me, ‘My grace is sufficient for you, for my power is made perfect in weakness.’ Therefore I will boast all the more gladly about my weaknesses, so that Christ's power may rest on me. That is why, for Christ's sake, I delight in weaknesses, in insults, in hardships, in persecutions, in difficulties. For when I am weak, then I am strong” (2 Cor. 12:7-10 NIV).
Remember that God is with you in every situation, no matter the pain or weakness—and will carry you through the pain.
Dr. Steven Burns, MD, is board-certified in family medicine and has been in practice for more than 30 years. Opinions are his own.